A requirement for the Anthem for SOCA Benefit Plan is to attach a completed Employer Application with the Sold Group submission. The Employer Application is only available on the HR Dashboard and should be completed by the HR Manager listed in FormFire for the company.
To access the Employer Application, select the Anthem SOCA ER Application button under Employer Medical Info.
The Employer Application is split into 8 sections. To learn more about a specific section, select a link below:
- Health Plan
- HSA Option
- Employer Information
- Eligibility
- Contribution Requirements
- Prior Coverage
- Review Terms and Conditions
- Signature
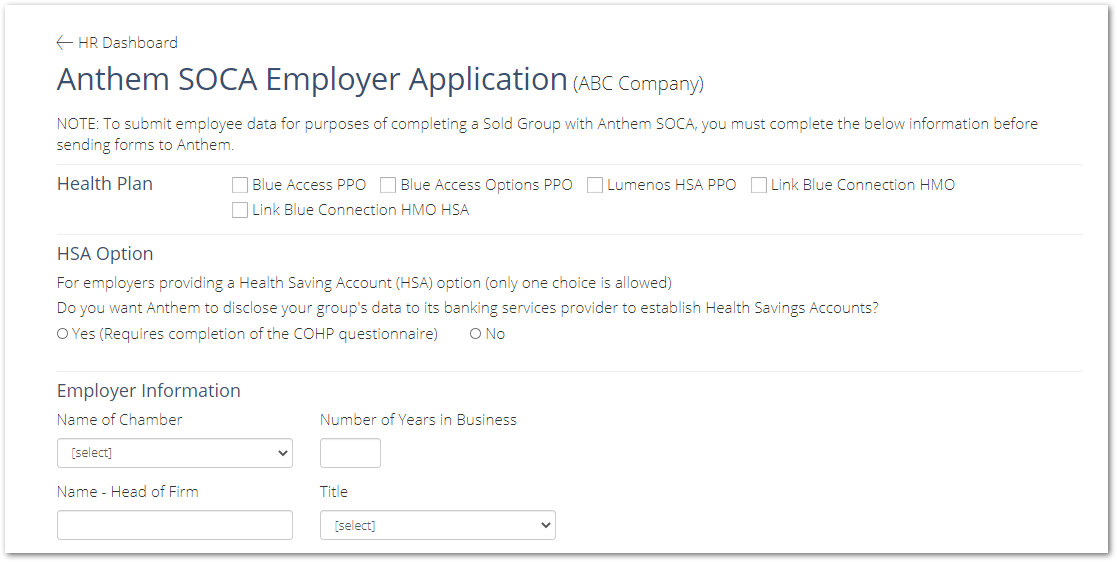
Health Plan
In this section, you'll be asked to select which health plan your company will be enrolling in with Anthem SOCA:
- Blue Access PPO
- Blue Access Options PPO
- Lumenos HSA PPO
- Link Blue Connections HMO
- Link Blue Connections HMO HSA
HSA Option
In this section, if your company is providing a Health Savings Account (HSA) option you'll be asked to answer Yes or No to the following question: Do you want Anthem to disclose your Group's data to its banking services provider to establish Health Savings Accounts?
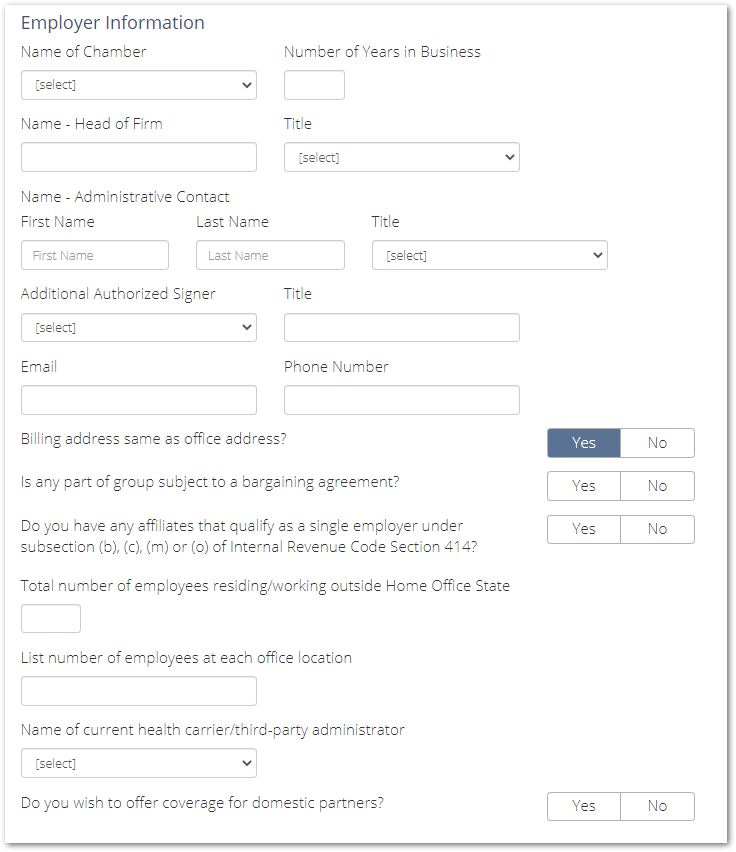
Employer Information
In this section, you'll be asked to answer questions, such as:
- Name of Chamber
- Head of Firm and Title
- Administrative Contact, Title
- Additional Authorized Signer and Title
- If subject to a bargaining agreement
- If subject to COBRA
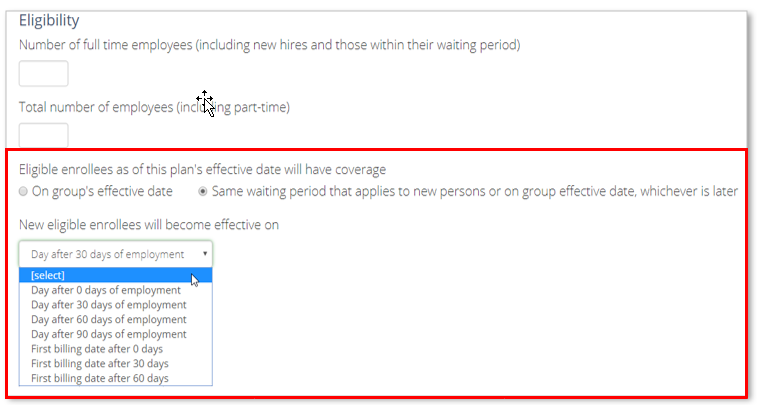
Eligibility
In this section, you'll be required to enter in the following information:
- Number of full time Employees
- Total number of Employees (including part-time)
- Effective date of coverage for eligible Employees
- When new eligible enrollees will become effective
- As the HR Manager, you must select the eligibility waiting period to indicate when benefits become effective for new Employees. Classes of Employee may not have different waiting periods under the SOCA Benefit Plan.
- Should your company want to change your waiting period, please contact Anthem and request the Ohio MEWA Administrative and Benefit Plan Change Authorization Form for instructions.
- If you are waiving the eligibility period for ALL existing Employees at the initial Group enrollment
- If you are a sole proprietor

Sole proprietors are eligible to participate in the SOCA Benefit Plan. However, due to regulator requirements, total sole proprietor membership cannot exceed 10% of the total membership of the plan.
Lastly, you'll be asked if you would like to authorize the agent/producer/broker/general agent whose name is attached to this application to use the EmployerAccess system of Anthem or Anthem Life Insurance Company to access the group’s information, such as but not limited to enrollees, plan selections, and bills/invoices. You'll only select the box noted below if you DO NOT want to grant this access.
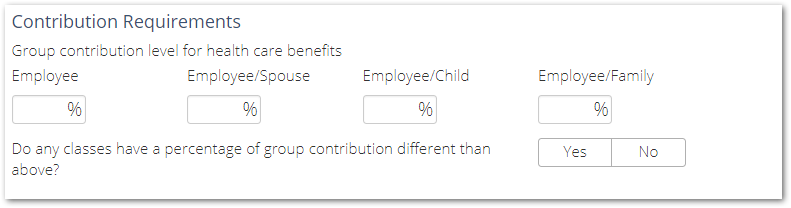
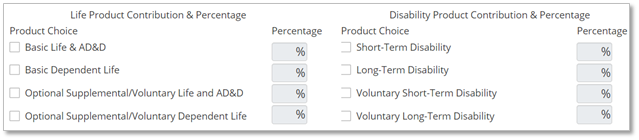
Contribution Requirements
In this section, you'll be asked to enter in the contributions that your company will make to the cost of the plan or plans offered. According to the Anthem Producer Guide, the minimum Employer contribution is:
- At least 50% of the total cost for health benefits in the event the Employee has single benefits
- At least 25% of the total cost for health benefits chosen in the event the Employee has dependent benefits
- Failing to enter the correct Employer contributions will result in an error.
The Anthem for SOCA Benefit Plan recommends Employers establish rates for single and family rates to avoid discrimination.
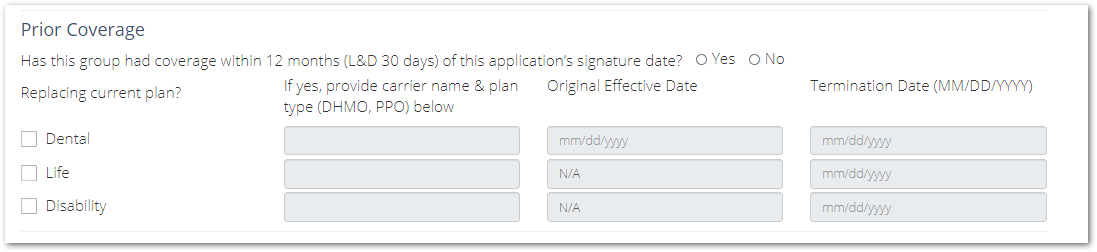
Prior Coverage
In this section, you'll be asked to enter in any prior coverage offered to your Employees in the last 12 months and if any current plans will be replaced.
Review Terms and Conditions
In this section, you'll review the terms and conditions. Make sure to scroll through all items listed in this section.

Signature
If you skip an entire section or even 1 question, you won't have the ability to sign the Employer Application.
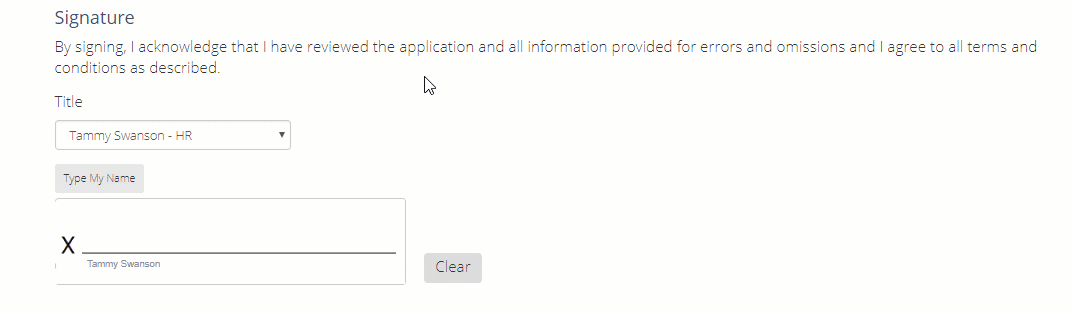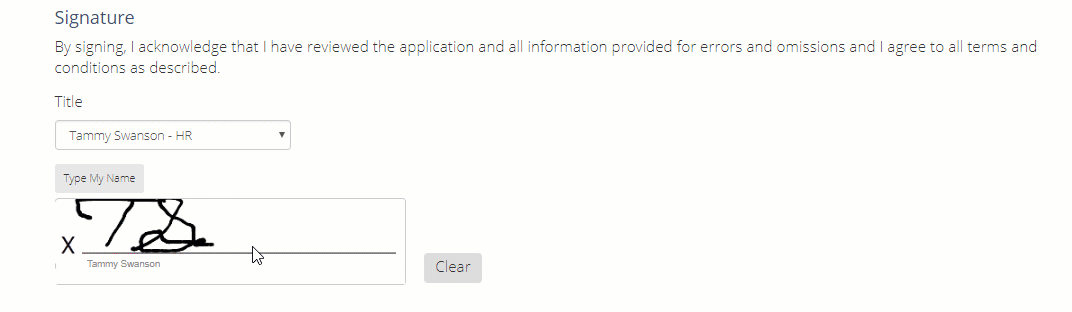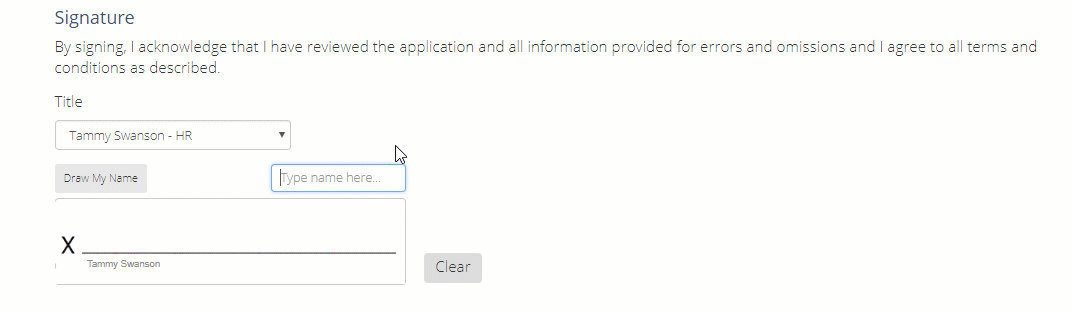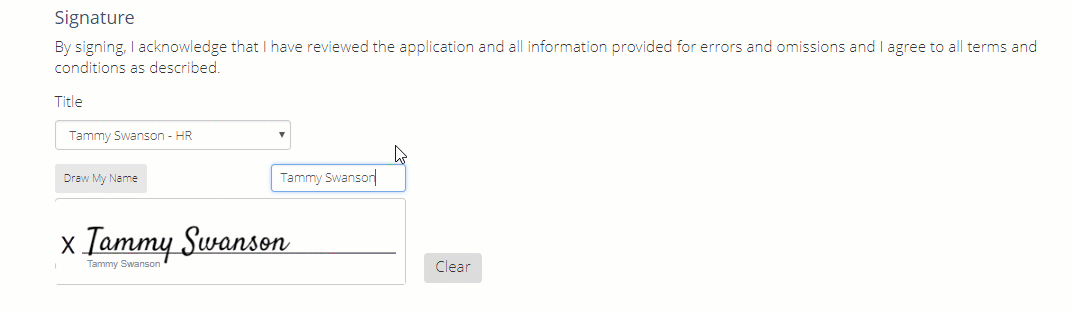
Once the entire application has been completed, you can either type or draw your signature in this area.
Once all items have been completed, select the Save button at the bottom left-hand side of the screen. doing this will ensure that the Employer Application has been completed and ready for your Insurance Broker to send directly to Anthem.
NOTE: Any changes to the information in the Employer Application will require a new signature.

Comments
0 comments
Article is closed for comments.